Bridging between worlds in Switzerland - the promise of transcultural psychiatry

In 2015, when Amadou, a fifteen-year-old Guinean boy, reached Switzerland, he was hospitalized with strong antipsychotic medications. He had developed life-threatening depression, suicidal behavior, and severe bouts of psychosis.
Just five years later, in 2020, his life is strikingly different. He has made many friends, goes to work every day, and can afford to live in his own flat. He says the reason is his psychiatrist, who delivers culturally appropriate mental health care for migrants, also known as ‘transcultural psychiatry’.
This article is part of Changing the Narrative. Articles in this series are written by student or early career journalists who took part in The Local's training course on solutions-focused migration reporting. Find out more about the project here.
"My psychiatrist saved my life," says Amadou. "Before him, I wanted to commit suicide, and without him, I would not be speaking with you right now.
"If I had to tell you everything he’s done for me, we would end up speaking all night. He helped me find a job, get my driver’s license, and most importantly, he gave me the courage to call my mother for the first time in three years."
Amadou’s story reflects the rough reality that many migrants face as they reach places like Switzerland, the country with the largest share of migrants in the whole of Europe.
MORE IN THIS SERIES:
Despite being one of the richest countries in the world, there is "clear evidence" that some migrant populations, especially refugees and undocumented migrants, still struggle to enjoy the same quality of mental health as the rest of the Swiss population, warns Denise Efionayi from Neuchatel University, who co-authored the country’s latest report on migration.
While massive disparities have existed for years, local tools that could bridge the gap, including culturally appropriate psychiatry services, are not yet mainstream - even though they have run for over two decades in Switzerland.
Shedding light on such life-saving services seems more critical than ever, especially as coronavirus-imposed restrictions batter mental health services and exacerbate existing inequalities.

Photo: Appartenances
Transcultural psychiatry: A bridge between two worlds
Transcultural psychiatry is a sub-branch of psychiatry that responds to the diverse cultural backgrounds that migrants have, as well as their life experiences that can sometimes include abuse, torture and war.
"Transcultural psychiatry is a sub-speciality of psychiatry that acknowledges the cultural background of patients, and adapts to work within the patient’s framework of health and disease, rather than imposing a Western view of psychiatry on the patient," explains Dr. Felicia Dutray, who is at the helm of transcultural psychiatry services at Appartenances, an NGO in Lausanne partially funded by the Canton of Vaud.
"If a patient believes that his mental health condition is due to bad spirits, we don't judge him for it," she adds. "Instead, we acknowledge that his framework is valid, and try to understand what it means for him so that we can work with it."
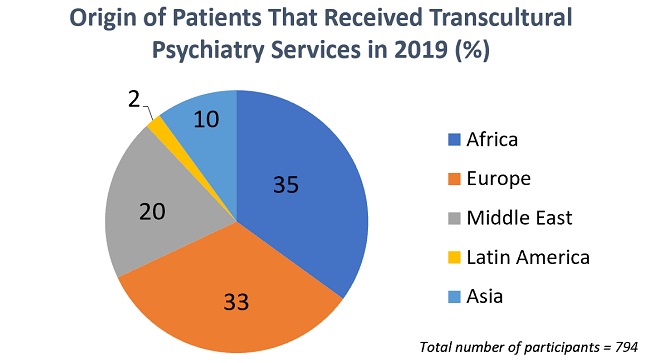
For almost three decades, Appartenances has catered to the mental health needs of migrants in the French-speaking part of Switzerland, receiving nearly 800 patients a year. Like all psychotherapy in Switzerland, services are paid for by insurance companies.
During most sessions, Dutray is assisted by professional interpreters to overcome potential language barriers, or to help the patient understand the aims of psychiatry and psychology, which are Western concepts sometimes unfamiliar to patients.
After two decades of working in the field, she is convinced that transcultural psychiatry benefits patients.
"People feel relieved after sessions, and they keep coming in, sometimes for several years," she notes. "In many cases, people’s symptoms even reduce, and this is clear from our internal evaluations with patient questionnaires before and after sessions."
One of the co-founders of Appartenances, Dr. Jean-Claude Métraux prefers to avoid using the term "transcultural". Instead, he refers to his work as "bridging between the worlds of patients and doctors".
Although Métraux is no longer officially affiliated with Appartenances, he still delivers training sessions on migrant mental health for the NGO. In 2019, 1,400 people received some form of training, most of them social workers and health professionals, as well as interpreters.
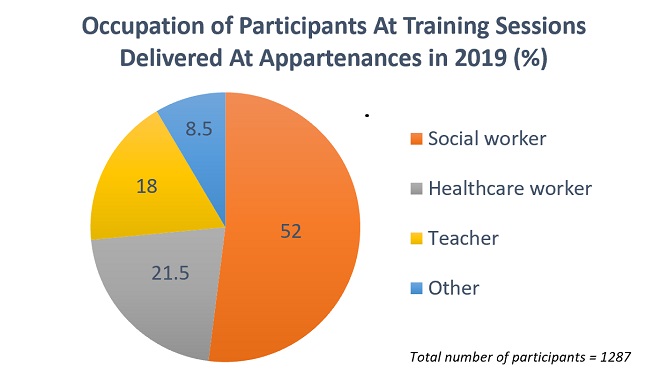
Apart from delivering training, Métraux also runs his own private clinic. Like Dutray, he is a strong believer that therapy must extend beyond the realms of the consultation room. Sometimes, this may involve getting in touch with lawyers and social workers to help patients with legal paperwork, or even finding a flat.
"The idea is to go further than the office, and to foster participatory collectives where people feel recognized in a nurturing environment," says Métraux.
It is perhaps not a coincidence that Appartenances also offers social spaces for children and adults, three of which are exclusive to women. These collectives help migrants build their own networks, become autonomous, and integrate into society through a range of fun and useful activities, including art workshops, French classes, or even IT skills.

Photo: Appartenances
Recognising patients as equals
Establishing mutual recognition with patients is crucial, says Métraux as he reflects on his work.
He argues that, before any diagnosis can be made, doctors must first establish "mutual recognition" with patients and understand the social, political, cultural and juridical context that often shapes their health.
His comment is particularly pertinent given mounting evidence that migrants are often misdiagnosed, precisely because psychiatrists miss important contextual details during consultations. As a result, the quality of care they receive takes a big hit, studies show.
Discrimination, for instance, can trigger an auto-exclusion syndrome that is sometimes confused with psychosis in migrant populations, he adds. But once patients are recognized as equals by their doctors, their psychiatric symptoms can even attenuate in some cases, says Métraux.
"A lack of recognition is a deep-seated problem in society that exacerbates mental health issues of migrants," he says. "This is why it’s so important to offer patients a context where they feel recognized, in the clinic and also outside the clinic."
While his emphasis on mutual recognition may seem far-fetched to some, it is consistent with data on discrimination and mental health in Switzerland. Migrants that make it to Switzerland are more lonely, and three times as likely to experience discrimination, in comparison to locals without a migration background, says the Federal Office of Public Health.
"We know that mental health and discrimination correlate quite strongly in some migrant populations, but not all," adds Efionayi.
Métraux emphasizes that mutual recognition can only be established when difference is seen as an asset, rather than a deficit. He also warns against labelling migrants as ‘vulnerable’ because it implies that others are invulnerable, thus creating the power asymmetries he is so motivated to break down.
In his sessions, he even goes as far as to share his own vulnerabilities to forge a bond with his patients. He also works hard to empower his patients to recognize their capacities, and their inherent ability to take control of their lives.
"To treat each other as equals, we need to show our vulnerability as doctors, and stop seeing difference as a deficit, as it is commonly done."
Stockholm’s promising approach to migrant mental health: 'Mainstreaming'
Switzerland’s example is just the tip of the iceberg when it comes to delivering culturally appropriate services for migrants, refugees and asylum seekers.
Up north in Sweden, where migrants make up about 20 percent of the overall population, Stockholm’s Transcultural Centre has catered to the needs of migrants for over two decades, says Dr. Sofie Bäärnhielm, a leading psychiatrist, and director of the centre since the early 2000s.
She says the Transcultural Centre fills the vacuum of expertise in migration and health, especially in medical schools, where there is "very little" training in cross-cultural services.
Unlike Switzerland’s Apartenances, The Transcultural Centre operates exclusively as a knowledge centre that offers support and training in the field of migration and mental health, especially for asylum seekers, refugees or undocumented migrants.
MORE IN THIS SERIES:
During training sessions, one of the Centre’s favorites is the cultural formulation questionnaire, which is routinely used around the world by healthcare and social workers to better understand a migrant’s context, including at Appartenances. It was designed in North America, and incorporated into the fifth iteration of the Diagnostic Statistical Manual for Mental Disorders (DSM) several years ago.
When it comes to training, the Centre’s approach is rather special, as it extends beyond psychiatrists, health professionals or social workers - it also strives to train teachers, workplaces, churches, NGOs, or anyone else that is interested in migrant health, says Bäärnhielm.
In fact, the Centre’s mission is to "mainstream" cross-cultural skills into Swedish society so that it becomes responsive to the diverse needs of migrants.
"Our mission is to embed cross-cultural skills into Swedish society, as migrants don’t just interact with healthcare," she says. "They interact with the whole of society, and that’s why the whole of society must become more responsive to their diverse needs."
Mainstreaming cross-cultural skills across all sectors is a particularly important strategy, comments Dr. Inka Weissbecker, a WHO expert in mental health. She says it could take the edge off overwhelmed mental health services, and also prevent migrants from having to see a psychiatrist in the first place. She explains that such whole-of-society approaches can make mental health support and care more widely available and accessible, while also addressing some of the root causes of poor mental health.
In 2019, the Transcultural Centre trained over 4,200 people, including healthcare workers in outpatient clinics, nursing wards, as well as workplaces and NGOs, among others. Since the coronavirus struck, the centre has maintained its efforts, albeit through Zoom, with funding from Stockholm’s authorities.

Photo: Appartenances
No perfect solutions
Although Amadou’s life has taken a new turn since he began therapy, since he began cross-cultural therapy, it doesn’t work for everyone, and outcomes may depend on a migrant’s context, which can be highly dynamic, warns Dutray. She notes that an unsuccessful asylum request can have devastating effects on mental health, irrespective of a psychiatrist’s calibre or the length of therapy.
Local evaluations of transcultural psychiatry services are also difficult to achieve, mainly because they are expensive and logistically complex to conduct - especially for NGOs like Appartenances, she adds. Even when resources are available, it can be difficult to recruit patients, notes Dutray. “If you don’t know where you’re sleeping or don’t have papers, you’re unlikely to take part in a study.
On the upside, one robust evaluation of a cultural consultation service in 100 patients showed that it can respond to the needs of diverse populations, improve diagnosis and treatment outcomes. The evaluation was published in the Canadian Journal of Psychiatry, and is one of many that have been produced in the past seventy years since transcultural psychiatry was developed.

Amadou was hospitalised when he arrived in Switzerland as a 15-year-old. Photo: Private
Although today, transcultural psychiatrists have access to robust questionnaires like the cultural formulation questionnaire, the original English version must be translated and adapted for different contexts - and this requires considerable expertise that is not always available, warns Bäärnhielm. She recounts when the questionnaire was first introduced to Sweden, and how difficult it was to translate concepts like "race", which is a controversial term in Sweden, and to make sure that the translated questionnaire was useful for its users.
Funding is another issue, as delivering specialized mental health services for migrants is "not exactly lucrative", so there is little incentive to pay for high-quality training or research, said a Swiss expert familiar with the topic, who asked to stay anonymous.
"Transcultural psychiatry is a totally different ball game compared to having a profitable private clinic for patients that can afford to pay," said the expert. "As a result, transcultural psychiatry curricula are limited, there is a lack of high-quality training, and systematic evaluations of effectiveness are also scarce, as nobody will pay for it."
In Sweden, culture-responsive mental health services are also the exception rather than the rule because there is simply not enough interest, says Bäärnhielm. One way forward, she suggests, could involve strengthening migrant health advocacy, as it is still fragmented and resource-poor.
Following his undergraduate studies in biology, Svĕt Lustig shifted gears to study public health at the London School of Tropical Hyigene and Medicine, alongside weekly reporting for Health Policy Watch, an open-access news service based in Geneva. He was born in Switzerland, and is half-Czech and half-Indian.
Comments
See Also
Just five years later, in 2020, his life is strikingly different. He has made many friends, goes to work every day, and can afford to live in his own flat. He says the reason is his psychiatrist, who delivers culturally appropriate mental health care for migrants, also known as ‘transcultural psychiatry’.
This article is part of Changing the Narrative. Articles in this series are written by student or early career journalists who took part in The Local's training course on solutions-focused migration reporting. Find out more about the project here.
"My psychiatrist saved my life," says Amadou. "Before him, I wanted to commit suicide, and without him, I would not be speaking with you right now.
"If I had to tell you everything he’s done for me, we would end up speaking all night. He helped me find a job, get my driver’s license, and most importantly, he gave me the courage to call my mother for the first time in three years."
Amadou’s story reflects the rough reality that many migrants face as they reach places like Switzerland, the country with the largest share of migrants in the whole of Europe.
Despite being one of the richest countries in the world, there is "clear evidence" that some migrant populations, especially refugees and undocumented migrants, still struggle to enjoy the same quality of mental health as the rest of the Swiss population, warns Denise Efionayi from Neuchatel University, who co-authored the country’s latest report on migration.
While massive disparities have existed for years, local tools that could bridge the gap, including culturally appropriate psychiatry services, are not yet mainstream - even though they have run for over two decades in Switzerland.
Shedding light on such life-saving services seems more critical than ever, especially as coronavirus-imposed restrictions batter mental health services and exacerbate existing inequalities.

Photo: Appartenances
Transcultural psychiatry: A bridge between two worlds
Transcultural psychiatry is a sub-branch of psychiatry that responds to the diverse cultural backgrounds that migrants have, as well as their life experiences that can sometimes include abuse, torture and war.
"Transcultural psychiatry is a sub-speciality of psychiatry that acknowledges the cultural background of patients, and adapts to work within the patient’s framework of health and disease, rather than imposing a Western view of psychiatry on the patient," explains Dr. Felicia Dutray, who is at the helm of transcultural psychiatry services at Appartenances, an NGO in Lausanne partially funded by the Canton of Vaud.
"If a patient believes that his mental health condition is due to bad spirits, we don't judge him for it," she adds. "Instead, we acknowledge that his framework is valid, and try to understand what it means for him so that we can work with it."
For almost three decades, Appartenances has catered to the mental health needs of migrants in the French-speaking part of Switzerland, receiving nearly 800 patients a year. Like all psychotherapy in Switzerland, services are paid for by insurance companies.
During most sessions, Dutray is assisted by professional interpreters to overcome potential language barriers, or to help the patient understand the aims of psychiatry and psychology, which are Western concepts sometimes unfamiliar to patients.
After two decades of working in the field, she is convinced that transcultural psychiatry benefits patients.
"People feel relieved after sessions, and they keep coming in, sometimes for several years," she notes. "In many cases, people’s symptoms even reduce, and this is clear from our internal evaluations with patient questionnaires before and after sessions."
One of the co-founders of Appartenances, Dr. Jean-Claude Métraux prefers to avoid using the term "transcultural". Instead, he refers to his work as "bridging between the worlds of patients and doctors".
Although Métraux is no longer officially affiliated with Appartenances, he still delivers training sessions on migrant mental health for the NGO. In 2019, 1,400 people received some form of training, most of them social workers and health professionals, as well as interpreters.

Apart from delivering training, Métraux also runs his own private clinic. Like Dutray, he is a strong believer that therapy must extend beyond the realms of the consultation room. Sometimes, this may involve getting in touch with lawyers and social workers to help patients with legal paperwork, or even finding a flat.
"The idea is to go further than the office, and to foster participatory collectives where people feel recognized in a nurturing environment," says Métraux.
It is perhaps not a coincidence that Appartenances also offers social spaces for children and adults, three of which are exclusive to women. These collectives help migrants build their own networks, become autonomous, and integrate into society through a range of fun and useful activities, including art workshops, French classes, or even IT skills.

Photo: Appartenances
Recognising patients as equals
Establishing mutual recognition with patients is crucial, says Métraux as he reflects on his work.
He argues that, before any diagnosis can be made, doctors must first establish "mutual recognition" with patients and understand the social, political, cultural and juridical context that often shapes their health.
His comment is particularly pertinent given mounting evidence that migrants are often misdiagnosed, precisely because psychiatrists miss important contextual details during consultations. As a result, the quality of care they receive takes a big hit, studies show.
Discrimination, for instance, can trigger an auto-exclusion syndrome that is sometimes confused with psychosis in migrant populations, he adds. But once patients are recognized as equals by their doctors, their psychiatric symptoms can even attenuate in some cases, says Métraux.
"A lack of recognition is a deep-seated problem in society that exacerbates mental health issues of migrants," he says. "This is why it’s so important to offer patients a context where they feel recognized, in the clinic and also outside the clinic."
While his emphasis on mutual recognition may seem far-fetched to some, it is consistent with data on discrimination and mental health in Switzerland. Migrants that make it to Switzerland are more lonely, and three times as likely to experience discrimination, in comparison to locals without a migration background, says the Federal Office of Public Health.
"We know that mental health and discrimination correlate quite strongly in some migrant populations, but not all," adds Efionayi.
Métraux emphasizes that mutual recognition can only be established when difference is seen as an asset, rather than a deficit. He also warns against labelling migrants as ‘vulnerable’ because it implies that others are invulnerable, thus creating the power asymmetries he is so motivated to break down.
In his sessions, he even goes as far as to share his own vulnerabilities to forge a bond with his patients. He also works hard to empower his patients to recognize their capacities, and their inherent ability to take control of their lives.
"To treat each other as equals, we need to show our vulnerability as doctors, and stop seeing difference as a deficit, as it is commonly done."

Stockholm’s promising approach to migrant mental health: 'Mainstreaming'
Switzerland’s example is just the tip of the iceberg when it comes to delivering culturally appropriate services for migrants, refugees and asylum seekers.
Up north in Sweden, where migrants make up about 20 percent of the overall population, Stockholm’s Transcultural Centre has catered to the needs of migrants for over two decades, says Dr. Sofie Bäärnhielm, a leading psychiatrist, and director of the centre since the early 2000s.
She says the Transcultural Centre fills the vacuum of expertise in migration and health, especially in medical schools, where there is "very little" training in cross-cultural services.
Unlike Switzerland’s Apartenances, The Transcultural Centre operates exclusively as a knowledge centre that offers support and training in the field of migration and mental health, especially for asylum seekers, refugees or undocumented migrants.
During training sessions, one of the Centre’s favorites is the cultural formulation questionnaire, which is routinely used around the world by healthcare and social workers to better understand a migrant’s context, including at Appartenances. It was designed in North America, and incorporated into the fifth iteration of the Diagnostic Statistical Manual for Mental Disorders (DSM) several years ago.
When it comes to training, the Centre’s approach is rather special, as it extends beyond psychiatrists, health professionals or social workers - it also strives to train teachers, workplaces, churches, NGOs, or anyone else that is interested in migrant health, says Bäärnhielm.
In fact, the Centre’s mission is to "mainstream" cross-cultural skills into Swedish society so that it becomes responsive to the diverse needs of migrants.
"Our mission is to embed cross-cultural skills into Swedish society, as migrants don’t just interact with healthcare," she says. "They interact with the whole of society, and that’s why the whole of society must become more responsive to their diverse needs."
Mainstreaming cross-cultural skills across all sectors is a particularly important strategy, comments Dr. Inka Weissbecker, a WHO expert in mental health. She says it could take the edge off overwhelmed mental health services, and also prevent migrants from having to see a psychiatrist in the first place. She explains that such whole-of-society approaches can make mental health support and care more widely available and accessible, while also addressing some of the root causes of poor mental health.
In 2019, the Transcultural Centre trained over 4,200 people, including healthcare workers in outpatient clinics, nursing wards, as well as workplaces and NGOs, among others. Since the coronavirus struck, the centre has maintained its efforts, albeit through Zoom, with funding from Stockholm’s authorities.

Photo: Appartenances
No perfect solutions
Although Amadou’s life has taken a new turn since he began therapy, since he began cross-cultural therapy, it doesn’t work for everyone, and outcomes may depend on a migrant’s context, which can be highly dynamic, warns Dutray. She notes that an unsuccessful asylum request can have devastating effects on mental health, irrespective of a psychiatrist’s calibre or the length of therapy.
Local evaluations of transcultural psychiatry services are also difficult to achieve, mainly because they are expensive and logistically complex to conduct - especially for NGOs like Appartenances, she adds. Even when resources are available, it can be difficult to recruit patients, notes Dutray. “If you don’t know where you’re sleeping or don’t have papers, you’re unlikely to take part in a study.
On the upside, one robust evaluation of a cultural consultation service in 100 patients showed that it can respond to the needs of diverse populations, improve diagnosis and treatment outcomes. The evaluation was published in the Canadian Journal of Psychiatry, and is one of many that have been produced in the past seventy years since transcultural psychiatry was developed.

Amadou was hospitalised when he arrived in Switzerland as a 15-year-old. Photo: Private
Although today, transcultural psychiatrists have access to robust questionnaires like the cultural formulation questionnaire, the original English version must be translated and adapted for different contexts - and this requires considerable expertise that is not always available, warns Bäärnhielm. She recounts when the questionnaire was first introduced to Sweden, and how difficult it was to translate concepts like "race", which is a controversial term in Sweden, and to make sure that the translated questionnaire was useful for its users.
Funding is another issue, as delivering specialized mental health services for migrants is "not exactly lucrative", so there is little incentive to pay for high-quality training or research, said a Swiss expert familiar with the topic, who asked to stay anonymous.
"Transcultural psychiatry is a totally different ball game compared to having a profitable private clinic for patients that can afford to pay," said the expert. "As a result, transcultural psychiatry curricula are limited, there is a lack of high-quality training, and systematic evaluations of effectiveness are also scarce, as nobody will pay for it."
In Sweden, culture-responsive mental health services are also the exception rather than the rule because there is simply not enough interest, says Bäärnhielm. One way forward, she suggests, could involve strengthening migrant health advocacy, as it is still fragmented and resource-poor.
Following his undergraduate studies in biology, Svĕt Lustig shifted gears to study public health at the London School of Tropical Hyigene and Medicine, alongside weekly reporting for Health Policy Watch, an open-access news service based in Geneva. He was born in Switzerland, and is half-Czech and half-Indian.
Join the conversation in our comments section below. Share your own views and experience and if you have a question or suggestion for our journalists then email us at [email protected].
Please keep comments civil, constructive and on topic – and make sure to read our terms of use before getting involved.
Please log in here to leave a comment.