German court scraps ban on assisted suicide

Germany's highest court on
Wednesday ruled that a 2015 law banning professional assisted suicide was unconstitutional, as it robbed terminally ill patients of "the right to a self-determined death".
Judge Andreas Vosskuhle said the right included "the freedom to take one's life and seek help doing so".
The ruling is a major victory for the terminally ill patients, doctors and assisted suicide organisations who brought the case, complaining that the existing law went too far.
Known as Paragraph 217, the 2015 legislation penalised anyone offering assisted suicide as a professional service, whether they accepted payment or not.
READ ALSO: German court discusses legality of assisted suicide
It was mainly aimed at barring associations dedicated to supporting patients wanting to end their lives, but also meant medical personnel faced prosecution for prescribing life-terminating drugs.
The legal uncertainty worsened when a 2017 lower court ruled that officials could not refuse lethal medication in extreme cases, creating confusion among doctors.
The verdict on Wednesday from the Karlsruhe-based court was closely watched in a fast-ageing country where Catholic and Protestant Churches still exerts strong influence, but polls show growing public support for physician-assisted suicide.
It is also a particularly sensitive subject in Germany as the Nazis used what they euphemistically called "euthanasia" to exterminate around 200,000 disabled people.
"The right to live does not constitute an obligation to live," Wolfgang Putz, one of those who brought the case, told judges as they began the hearing last year.
READ ALSO: German court strengthens patients' rights in assisted suicide ruling
Patients' perspective
For Horst L., paragraph 217 closed a door. The media frenzy about the issue was too much for the cancer patient who wished to remain anonymous.
But in 2019 he read a personal statement before the Constitutional Court. L is suing because he is a member of the German Assisted Suicide Association, which gave him the green light in 2015 - all he had to do was give the signal.
But when the ban came into force, this became illegal. He therefore lost the peace of mind of knowing that if things got too tough, he could pull the plug.
He told the Süddeutsche Zeitung in 2018: "I find it outrageous when others tell me: you have to live, endure and accept."
Other patients, unable to receive assistance in Germany, traveled to neighbouring Switzerland, where assisted suicide is legal under certain conditions.
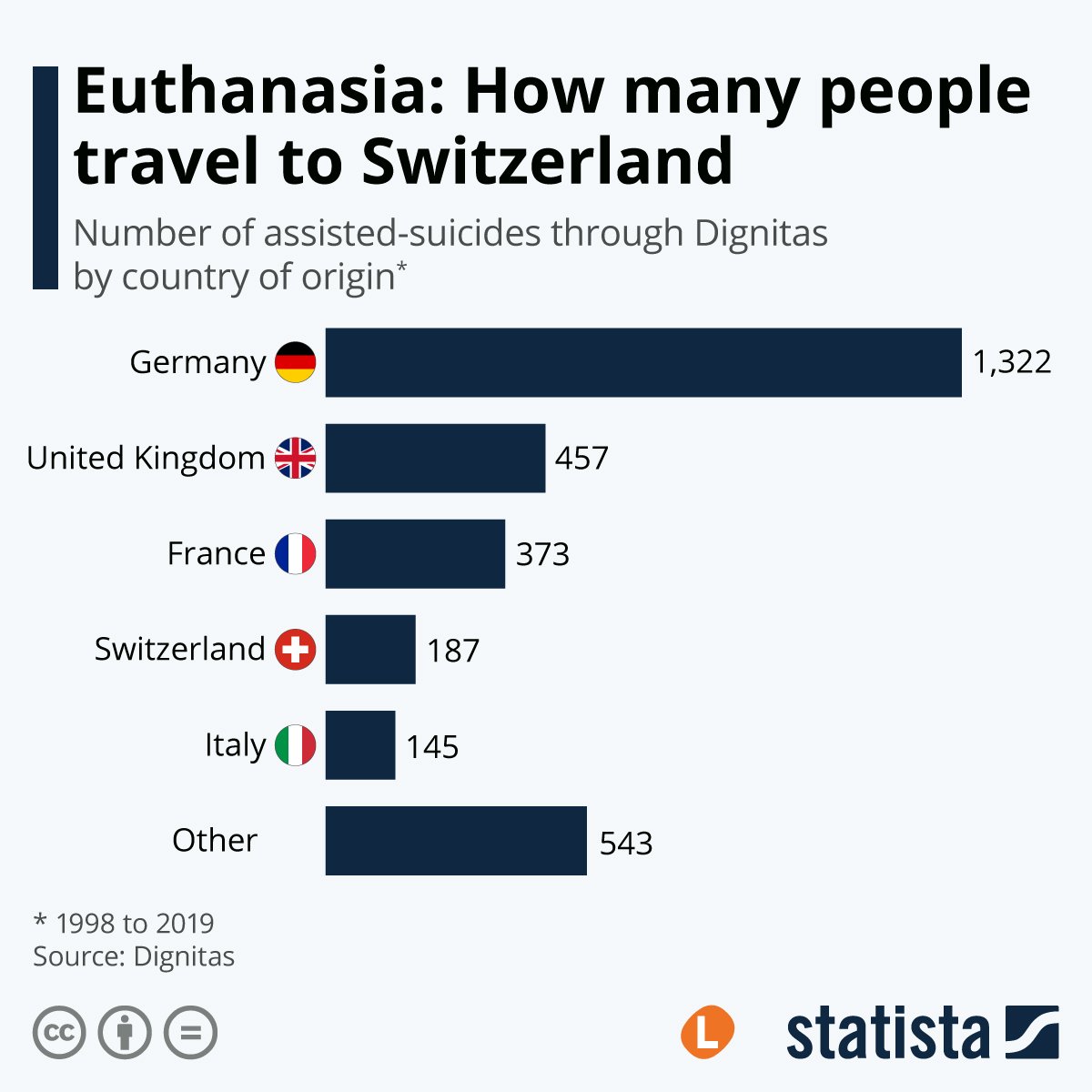
The following graph shows how many people traveled to Switzerland between 1998 and 2019 to receive suicide assistance from the non-profit Dignitas. Graph prepared for The Local by Statista.
Helmut Feldmann witnessed both his father and sister suffer painful deaths from lung disease COPD. Now he is ill himself and had made provisions for his death.
But since 2015, his membership to the Assisted Suicide Association has become worthless. “I do not accept that a few hundred parliamentarians are able to decide how I will die”, he told Der Spiegel before the verdict. “I will fight to the end”.
For other claimants the judgement has come too late. They have already lost their race against death during the lengthy procedural process.
Right to dignity
At the heart of the debate was the plaintiffs' argument that Germany's constitution guarantees personal freedom and dignity, which they said includes the right to a self-determined death.
For seriously ill patients who have chosen to end their life, the existing legislation made it "almost impossible to carry out that decision in a dignified manner", said Christoph Knauer, who represented two of the plaintiffs.
Under Paragraph 217, professionals falling foul of the law risked a fine and up to three years in prison.
This left German patients turning to family members or loved ones for help, some getting life-terminating medicine from abroad.
Judge Vosskuhle said Paragraph 217 "also violates the basic rights of persons and associations who wish to provide suicide assistance".
On the other side of the debate, the Catholic Church had objected to changing Paragraph 217.
Berlin's Archbishop Heiner Koch urged the court to "send a strong signal for the protection of lives".
The German Medical Association had likewise spoken out against legalising physician-assisted suicide.
Its former president Frank Ulrich Montgomery warned last year that if doctors were allowed to prescribe a cocktail of life-ending drugs, it could lead to legalising euthanasia -- where doctors take an active role in ending a patient's life, for instance through lethal injection.
Judge Vosskuhle acknowledged that the ruling would be a blow to supporters of Paragraph 217 but said the wishes of those wishing to end their lives had to be respected.
"We may regret their decision and try everything we can do change their minds but ultimately we must accept their freedom to choose," he said.
Euthanasia is officially legal in only three Europe Union countries -- the Netherlands, Belgium and Luxembourg -- but others allow or tolerate a form of assisted suicide.
In non-EU Switzerland, as well as in the US states of Vermont, Oregon and Washington, assisted suicide is legal.
A survey for broadcaster ARD on Tuesday found that 81 percent of Germans believed doctors should be allowed to help severely ill patients with their wish to die, up from 76 percent in 2012.
Sixty-seven percent of respondents said Germany's Paragraph 217 should be amended.
Comments
See Also
Judge Andreas Vosskuhle said the right included "the freedom to take one's life and seek help doing so".
The ruling is a major victory for the terminally ill patients, doctors and assisted suicide organisations who brought the case, complaining that the existing law went too far.
Known as Paragraph 217, the 2015 legislation penalised anyone offering assisted suicide as a professional service, whether they accepted payment or not.
READ ALSO: German court discusses legality of assisted suicide
It was mainly aimed at barring associations dedicated to supporting patients wanting to end their lives, but also meant medical personnel faced prosecution for prescribing life-terminating drugs.
The legal uncertainty worsened when a 2017 lower court ruled that officials could not refuse lethal medication in extreme cases, creating confusion among doctors.
The verdict on Wednesday from the Karlsruhe-based court was closely watched in a fast-ageing country where Catholic and Protestant Churches still exerts strong influence, but polls show growing public support for physician-assisted suicide.
It is also a particularly sensitive subject in Germany as the Nazis used what they euphemistically called "euthanasia" to exterminate around 200,000 disabled people.
"The right to live does not constitute an obligation to live," Wolfgang Putz, one of those who brought the case, told judges as they began the hearing last year.
READ ALSO: German court strengthens patients' rights in assisted suicide ruling
Patients' perspective
For Horst L., paragraph 217 closed a door. The media frenzy about the issue was too much for the cancer patient who wished to remain anonymous.
But in 2019 he read a personal statement before the Constitutional Court. L is suing because he is a member of the German Assisted Suicide Association, which gave him the green light in 2015 - all he had to do was give the signal.
But when the ban came into force, this became illegal. He therefore lost the peace of mind of knowing that if things got too tough, he could pull the plug.
He told the Süddeutsche Zeitung in 2018: "I find it outrageous when others tell me: you have to live, endure and accept."
Other patients, unable to receive assistance in Germany, traveled to neighbouring Switzerland, where assisted suicide is legal under certain conditions.

The following graph shows how many people traveled to Switzerland between 1998 and 2019 to receive suicide assistance from the non-profit Dignitas. Graph prepared for The Local by Statista.
Helmut Feldmann witnessed both his father and sister suffer painful deaths from lung disease COPD. Now he is ill himself and had made provisions for his death.
But since 2015, his membership to the Assisted Suicide Association has become worthless. “I do not accept that a few hundred parliamentarians are able to decide how I will die”, he told Der Spiegel before the verdict. “I will fight to the end”.
For other claimants the judgement has come too late. They have already lost their race against death during the lengthy procedural process.
Right to dignity
At the heart of the debate was the plaintiffs' argument that Germany's constitution guarantees personal freedom and dignity, which they said includes the right to a self-determined death.
For seriously ill patients who have chosen to end their life, the existing legislation made it "almost impossible to carry out that decision in a dignified manner", said Christoph Knauer, who represented two of the plaintiffs.
Under Paragraph 217, professionals falling foul of the law risked a fine and up to three years in prison.
This left German patients turning to family members or loved ones for help, some getting life-terminating medicine from abroad.
Judge Vosskuhle said Paragraph 217 "also violates the basic rights of persons and associations who wish to provide suicide assistance".
On the other side of the debate, the Catholic Church had objected to changing Paragraph 217.
Berlin's Archbishop Heiner Koch urged the court to "send a strong signal for the protection of lives".
The German Medical Association had likewise spoken out against legalising physician-assisted suicide.
Its former president Frank Ulrich Montgomery warned last year that if doctors were allowed to prescribe a cocktail of life-ending drugs, it could lead to legalising euthanasia -- where doctors take an active role in ending a patient's life, for instance through lethal injection.
Judge Vosskuhle acknowledged that the ruling would be a blow to supporters of Paragraph 217 but said the wishes of those wishing to end their lives had to be respected.
"We may regret their decision and try everything we can do change their minds but ultimately we must accept their freedom to choose," he said.
Euthanasia is officially legal in only three Europe Union countries -- the Netherlands, Belgium and Luxembourg -- but others allow or tolerate a form of assisted suicide.
In non-EU Switzerland, as well as in the US states of Vermont, Oregon and Washington, assisted suicide is legal.
A survey for broadcaster ARD on Tuesday found that 81 percent of Germans believed doctors should be allowed to help severely ill patients with their wish to die, up from 76 percent in 2012.
Sixty-seven percent of respondents said Germany's Paragraph 217 should be amended.
Join the conversation in our comments section below. Share your own views and experience and if you have a question or suggestion for our journalists then email us at [email protected].
Please keep comments civil, constructive and on topic – and make sure to read our terms of use before getting involved.
Please log in here to leave a comment.